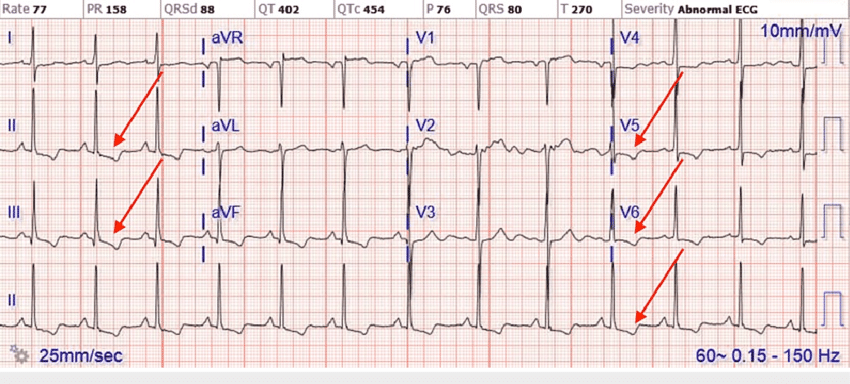
CC: CP - the NSTEMI
NSTEMI
The non-ST segment elevation myocardial infarction
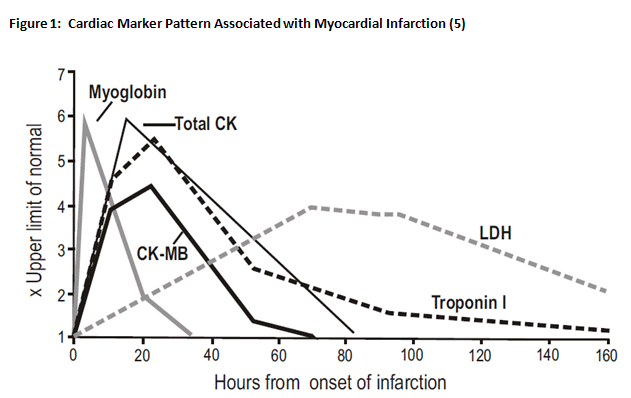
Back in MY early days, we were still using total CK and CK-MB and troponin was the new marker - from: Cardiac Troponin I (cTnI) New Generation Cardiac Marker of Choice. Graphical Representation-Levels of Cardiac Markers in AMI. http://www.tulipgroup.com/ Common_New/ Tech_Pubs_PDF/Cardiac.pdf.
Next, we turn to the non-ST elevated MI. By definition, this is a patient with an EKG that does not show ST elevation (hence the "non") but has evidence of cardiac cell death. This is an easy diagnosis nowadays with increasingly sensitive troponin tests, and it makes for another relatively easy admission disposition and treatment, such as…
NSTEMI should be treated with aspirin.
Heparin is the likely next step needed to prevent a thrombotic event. It would be best if you also utilized nitroglycerin as a vasodilator to keep the patient pain (and hopefully ischemia) free. Also, consider a beta-blocker to decrease the heart's workload.
To summarize, NSTEMIs are managed medically with ASA, NTG, Heparin, and Beta-blockers, but don't stop there.
Watch these patients closely. By definition, these are not going to the cath lab immediately, but they certainly could evolve into a cath lab activating STEMI. Also, consider calling your interventional cardiologist for any hemodynamically stable patient or even a patient whom you cannot control their symptoms (i.e. intractable pain/ischemia) despite maximum medical management. Unstable ventricular arrhythmias (v-tach) are definitely a cue to get on the phone with the cath lab.
Interestingly, I assume there is infarction after seeing a single elevated troponin, but the true definition of myocardial infarction is a 20% serial rise in troponin (at least according to prior standards). I am more familiar with Troponin I which should be repeated in 3 to 6 hours, but I have also worked at ERs that use 1-hour protocols with high-sensitivity troponin. Follow your hospital’s protocol.
Bottom Line: Follow your department’s protocol for utilizing troponin. It is unlikely that you will be making this decision on your own. Also, don’t lose the forest for the trees when an elevated troponin is found. There are other causes including myocardial hypoperfusion might not be ACS but a sick septic or anemic patient.
Despite these nuances, once that troponin is positive and a patient is placed in the NSTEMI bucket, the work-up and treatment is fairly straight forward. In my experience, the difficulties with CP arise with those patients who do not have any EKG or troponin abnormalities, and this is actually the majority of patients who come to the ER with chest pain!